A lengthy preamble:
The following post provides details of the day of the surgery and my two-day stay at the hospital.
I’m writing about my experience in hopes that others can benefit. I’m not a medical expert, this is not to advise you to have a myomectomy. Our bodies are different and it should be a personal decision made with medical consultation on how to treat/remove fibroids.
Additionally, I hope that anyone who feels like you are alone in your experience, will realize that you are not, and perhaps someone in your acquaintance has silently undergone the same thing. Don’t let anyone judge you for your decision. Also, if you are reading this, I hope you’re not squeamish.
Part 1: Myomectomy: The Prep
Read Time: 12 minutes
July 6th, 2018
Before the Surgery: We arrived almost an hour early for my check-in appointment. My parents were with me, they wanted to be there when I got out of surgery. Since I completed my check-in forms online the check-in process was easy. I added my mom’s phone number so she could receive text messages when my surgery commenced and completed. They tagged me and took us up some elevators to another set of waiting rooms.
Soon after I was called to do a vitals check, as well as height and weight. My blood pressure was on the high side, so they checked again on the other arm and it was fine. I was given my uniform for the surgery, along with instructions. “Take everything off, put the gown on, tie in back, put the PJs on tie in front, put the robe on open in front.”
“Everything?” I asked, I’m not even sure why. Of course I had to take off everything. But it was the fourth day of mensuration for me, so, even though it was a light day, I wasn’t prepared for the “everything off” instructions. So, everything came off and I dress in the clothes provided; for some reason I found it funny – it must have been the nerves catching up to me. But, here’s a thing you should be aware of, you take everything off when you’re doing a surgery. 
Next, I was lead to a waiting area that had a lot of curtained off sections. The nurse drew some blood (the first of MANY blood draws!) and inserted the IV catheter into my arm.
The doctors who were going to be involved in my surgery came by and introduced themselves. The anesthesiologist explained the process for the anesthesia and I signed papers for pain relief consent. In addition to the regular anesthesia, they would inject both sides of my abdomen with a pain relief drug (whose name I don’t remember) to help numb that area so I feel less pain after the surgery. However, if the pain was still unbearable after surgery, signing the consent form for an epidural before surgery would give them permission to administer it after surgery. Thankfully it didn’t come to that for me, but I figured it wouldn’t hurt to have a fallback. I received a shot to stop blood cloths, and waited for my time.
In the OR: After saying goodbye to my parents, I was taken up a few floors and down a few halls to the operating room. Let me take a moment here to say, this real life OR looked nothing like the ORs I saw on TV, for some reason it reminded me of a huge high-tech laundry room.
All I remember from the OR experience was taking everything except the gown off, lying down on the table while they placed blankets over me and telling the anesthesiologist that I often overheat when I am under covers. I remember her assuring me that they would be monitoring everything, her putting the drip into my IV, then nothing else.
Here is what I do know from the report, my questions, and the things connected to my body afterwards.
- They added another IV catheter to my left hand. I don’t know what drugs were going into that.
- I was intubated – I think this is normal practice for these types of things – and I was happy that I was completely out for this, I’ve seen people intubated and it does NOT look pleasant.
- A Foley catheter was inserted into my urethra – also happy I wasn’t wake for this.
- They cut through skin, ab muscles, and all the other layers to gain access to the uterus (avoiding bowel and bladder). The type of cut is known as a “bikini cut” which is horizontal, right above the pubic bone.
- One large fibroid was encountered that had to be removed, then two more (on stalks) were removed. Afterwards they looked for all the rest so they could figure out how to remove with the least amount of incisions (which I appreciate).
- Two incisions into the uterus were made to remove the two inside. Others were removed from around the uterus.
- I bled a lot, and they recycled some of my blood back to me (it calculates to almost a cup)
- After all the cutting I was stitched up again and checked that bleeding stopped.
- They removed the tube and gave me oxygen through a nasal cannula – I am assuming I had to respond to commands for them to remove the tube, but I do not recall this at all.
In Recovery: The first thing I remembered was waking up to people calling my name. The first thing I remember saying was that I was in pain. I was given the trigger to hold and told that I should press it to get the hydromorphone (which was a wonderful pain killer). I remember asking for pillows under my thighs because my legs felt really strange, then under my neck because that felt strange too. I also asked for more blankets because I was freezing. I remember asking all these things and just saying “thank you so much” every time someone came to my aid. I also remember asking a few times for the time. I remember them taking blood, I remember the blood pressure cuff automatically taking my blood pressure. I had compression boots to help with circulation.
I remember my parents sitting at my bedside and asking my dad to pull the covers up over my nose – like a ninja – because my nose was freezing. I remember being told that I might be nauseous, but I was feeling fine. I remember the doctor talking to me and telling me there were six big ones and showing me pictures. Then telling me she’ll see me the next day. Here I was a little confused. I swore the photos my mind saw were the fibroids in a bowl and the picture of my uterus taken from a position above my head, but when I saw the actual pictures the day after there were no photos like that.
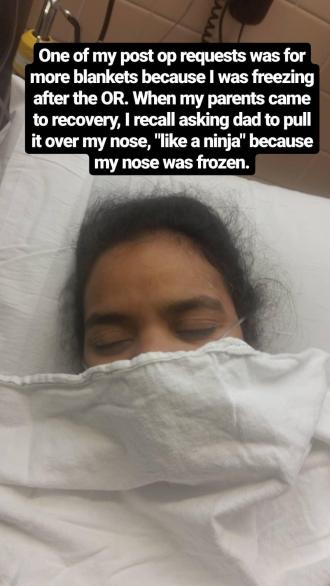
After a few minutes, the nurse attending asked how I was feeling and gave me some ice chips to chew. The ice chips went down without issue and I graduated to jello, which my parents fed to me because I was pretty cold and my hands were wrapped under four blankets.

Three of my friends dropped by while I was in recovery, to check on how I was doing. I remember saying whatever I wanted to say, but nothing completely out of the ordinary of what I would usually say – maybe just a little more cheerily. I remember being glad that I wasn’t more woozy and strange coming out of anesthesia.
By six I was placed in a room, I was able to shimmy over from the recovery bed to the room bed with some help. It was in the hospital bed that I became aware of the second IV catheter not hooked up to anything and the Foley catheter, which I couldn’t feel, but was aware of the tube running from out of me to a container hooked on the side of the bed. I had an injection to help with blood clots and another round of blood was drawn.
After my family and friends left, I tried to sleep, but I kept waking up whenever the staff came in to check on me. My nose was still really cold.
July 7th, 2018
Early the next morning they removed the Foley catheter and wanted me to try using the toilet. The removal itself was painless, the nurse deflated the balloon and it slid right out. Just before breakfast, when the nurse checked in on me, I had the urge to use the toilet, so she helped me get out of bed.
It was really difficult getting up out of bed, but I managed to push myself up, bracing with my arms, and stand. I was a very dizzy initially but managed to walk without much assistance. Here, I know I’m lucky because many women have a much harder time standing up and walking, especially less than 24-hrs after the surgery. Never attempt to get up unassisted the first time.
I had to urinate in this plastic container that they put in the toilet bowl called “the hat” (because of its shape) so that they could measure it, every time I went. Seriously, they are constantly measuring your urine.
I tried to have breakfast that day, but was unable to because I didn’t have much of an appetite. I drank some black coffee and ate the eggs, that was all I could manage in two hours. Because of my mobility, I was able to sit on a chair for most of the morning.
In packing for my stay, I brought two books and an iPad filled with Netflix downloads. I managed to watch two episodes of a sitcom, but otherwise I couldn’t concentrate on anything else.
My voice was still low, most likely due to the intubation, but I didn’t experience any soreness in my throat, I know that some people do, so that’s something else to note. I found it a little difficult to draw a really deep breath, it wasn’t that I couldn’t do it, but it felt like my insides were squishing together and hurting when I did. I was really sore.
There was more blood taken that day and I had to get a magnesium drip because my magnesium levels were low.
When lunch came around my appetite still hadn’t returned, so I spent two hours trying to eat as much as I could – which was not a lot. My parents came in to find me sitting with the tray in front of me around 2pm that day.
Later that evening, they disconnected me from the hydromorphone drip but left the two IV catheters in my arms. I was now free to walk around without pulling a pole with me. They gave me the lowest dosage of oxy for the pain.
One of my friends visited late that night and I walked around the corridors with her. Walking is very important in helping with recovery so I was determined to walk a few minutes each day, even though I was walking at a snail’s pace.
July 8th, 2018
I was running a low grade fever, additionally my heart rate was high and I was feeling anxious. It was the wee hours of the morning, but I got up and walked around the corridors a bit because I couldn’t sleep. My body started hurting, my left leg and my abdomen. The nurse didn’t think it was the pain meds, but in the morning I opted to take the ibuprofen instead of the oxy. The doctor on staff came around very early in the morning to check on me – I didn’t realize that they were so concerned about my heart rate. Other than the pain, anxiety and heart rate, I was more or less doing fine. More blood was taken for testing.

After the tests and the new painkiller, I finally slept and woke up feeling much better and completely famished. I was able to eat more of my breakfast that morning.
My doctor dropped in later that morning and gave me some bad news, my blood count was low after surgery – which was to be expected – but within the last 24-hrs it dropped even lower and they suggested a blood transfusion. I had stopped bleeding, so it wasn’t that I was losing any more blood, and a blood transfusion would mean staying in the hospital for an extra night. I didn’t want a transfusion, mostly I wanted to go home. So we agreed, I would get another blood test around 4pm that day, if the counts remained the same I could go home, however, if it dropped then the transfusion would be required not suggested.
My mom and two cousins came later that day, I told them the bad news, so they sat with me to wait it out. It was comforting having people with me, especially since I was starting to feel really sad that there was a possibility of staying another night. Additionally, even though it was lost in all of the other things happening, I had done only two of the “three Ps”, and I was concerned that I wouldn’t be able to go home because of that. “What are the three Ps?” you ask? Well, it’s peeing, pooping and passing gas. Basically they want to know that your digestive system is working well, with all the drugs, constipation and bloating are side effects.
Around 4pm, another blood test was taken and we sat around waiting for the results. The results came back and my count had rebounded, I did not absolutely need a transfusion, I could go home! The nurse gave me a few underpads and some hospital underwear to take home with me, I highly recommend these, ask your nurse when you are being released! I took a motrin and braced myself for the ride home.

I had a pillow to hold to my stomach which was so helpful, because the ride home was such a bumpy ride and I felt everything. It was so bumpy that I even bled a little – which was a tiny bit concerning as I had stopped bleeding.

When I arrived at home and was better able to examine myself I found a lot of black and blue, including the place on my arm where I received all the injections. Because of my iron and blood count, they told me not to take a shower until the afternoon of the following day, since it’s possible that the hot water could cause me to faint.

I was able to walk up and down the stairs, going really slowly and holding on to the banister. I was also able to get in and out of bed with only minimal struggle. I was happy to be home, but knew I had to settle in for the next six weeks. My daily pills were Ibuprofen, Colace, Gas-X, Iron and Vitamin C. More about these in the next post!
Pingback: Myomectomy: Afterwards | Eat. Read. Blog